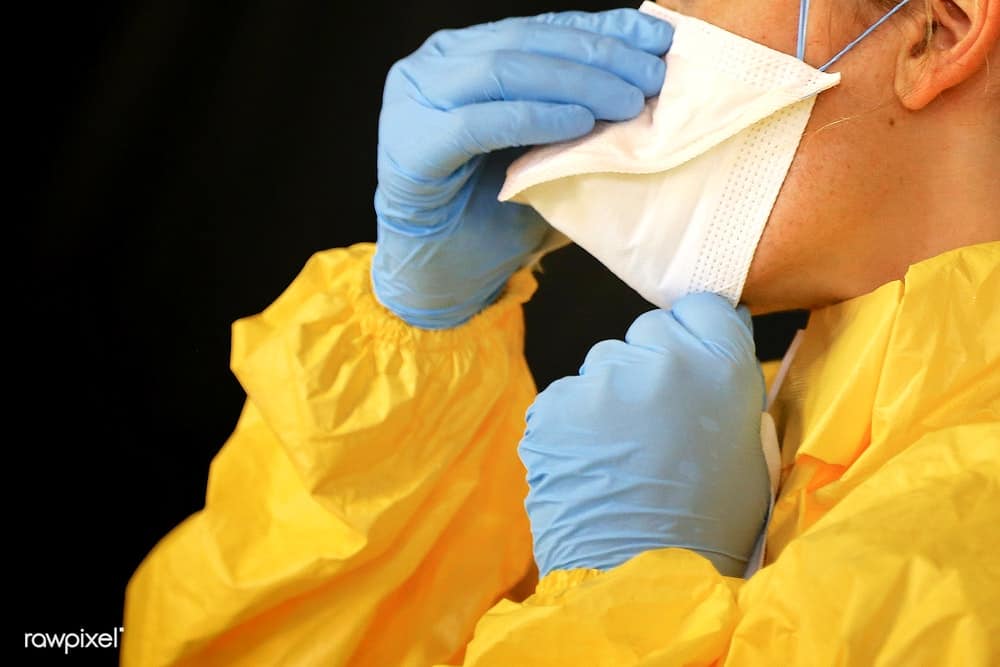
I want to explain why my medical colleagues and I feel so angry and frustrated about the protection offered to us by the government, and why a few of them are reluctant at the moment to look after Covid 19 patients.
All doctors , nurses and carers helping Covid positive patients need protective equipment. But as it turns out, the official advice was changed.
The British Medical Journal on March 14 had an article about what protective equipment we needed to wear if Covid 19 is suspected.
The rules were clear, that for Covid positive patients, as we
would for all very serious infections, we would need full PPE (Personal
Protective Equipment) – which means a filtering FFP3 facemask also called
“respirator“ which fits close to the persons face with elastic round ears, plus
a long sleeved gown, gloves and visor or other eye protection .
.
Yet, as the pandemic worsened, official guidance has changed, for pragmatic
and, perhaps, financial reasons.
All healthcare professionals have to see some patients without knowing whether they are Covid positive or not, because there isn’t enough testing. We also have to see patients who are definitely Covid positive – and get very close to them – without the full PPE.
As a result, we have a large number of our team off sick, some dangerously so.
Only last week, on March 28 – presumably for pragmatic reasons – Public Health England, and the four nations between them, agreed that Covid 19 should no longer be classified as a ‘high consequence infectious disease’. They therefore updated the guidance which meant that the full PPE would only be required “in Intensive Care Units or the hot zone of an Emergency Department”.
I should explain that a fluid repellent face mask is not the same as a visor or an FFP3 facemask. It’s a blue or green paper mask with folds and ties or elastic, which doesn’t sit snuggly on face so virus can get in or out. It is also called a surgical facemask. The visor is clear perplex attached to a headband.
A FFP3 facemask , also called a respirator fits quite snuggly to the face around the mouth and nose . The gown is long-sleeved, with elasticated wrists so there’s no skin exposed between gown sleeves and gloves. The apron is a flimsy plastic pinafore like a chef’s apron.
As a consequence of the new guidelines for PPE there will be more NHS staff off sick. It also means they will be replaced by retired staff, often elderly, who believe they will be getting full protection – but will not in fact get it.
That is why we will be burying our colleagues – because many people are not getting the basic equipment they should be getting. I don’t want to bury my friends.
I want to help – but I am not going to push myself forward until we get the proper filtering facemasks and full PPE.
I heard about the change of advice, and was given the letter, when I formally asked for filtering facemasks. There is a hotline number. I called it then got put through elsewhere, then was called back two days later, then spent some time being asked questions, by a very helpful woman.
When she understood that we were carrying out procedures that were putting us at risk, she offered me a box of ten.
I said it would last a couple of days only – the FFP3 facemasks last only four hours. She said she could not order more because the system would not allow it.
“What shall I do then?” I asked.
She suggested I put in a formal request every two days.
“Are you not supposed to be a hotline?” I said. She said she was very sorry – and I know she had done everything she could.
My colleagues are rigging up their own face masks where they can, out of acetate with holes punched with a hole puncher to thread the elastic of the paper surgical facemask through. I can’t believe they are as safe as they should be.
I feel a mixture of anger and anxiety – anger because one colleague is on oxygen and I am anxious for him, and for my husband with asthma. And because we are asking all these wonderful retired staff to come back and help us – not telling them they have changed the guidelines about what PPE they will get. Also, I’m also aware staff in care homes are given even less than the NHS.
Does it make sense to reduce the staff numbers in the NHS and the caring professions through sickness, let alone death, because of lack of Full Personal Protective Equipment, just at a time when we need all our staff and more? Does it make sense for these staff to become super spreaders of Covid 19 for the few days before they get symptoms, or longer if they are asymptomatic?